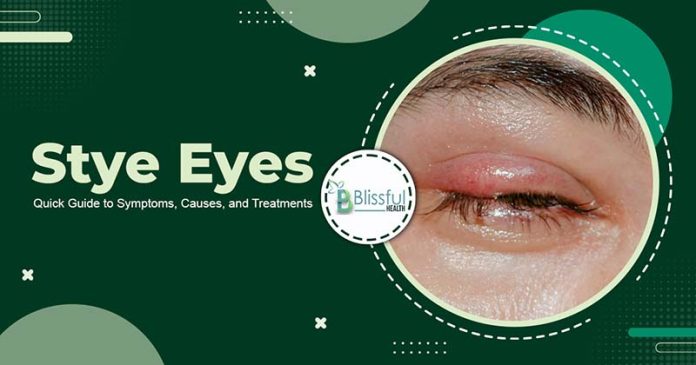
Let’s talk about stye eyes – those annoying, painful bumps that can show up on the edge of your eyelid. Just like a pimple, a stye, also known as a stye eye, happens when a small oil gland near your eyelashes gets all clogged up and infected. They’re pretty common, and while many can be dealt with at home, some might need a pro’s help from an eye care provider.
Overview Stye Eyes
A stye is a painful, red bump on the edge of your eyelid, resembling an acne pimple and tender to touch. It develops when an oil-producing gland in the eyelash follicle or eyelid skin is blocked, leading to a bacterial infection. Medically, a stye is known as a ‘hordeolum.’
Styes usually affect one eyelid but can appear on both. They typically last one to two weeks and resolve independently, but persistent styes may need medical intervention, possibly involving drainage and antibiotics.
Note that a stye differs from a chalazion, which forms farther back on the eyelid, is usually painless, and does not result from a bacterial infection. However, both conditions are treated similarly.
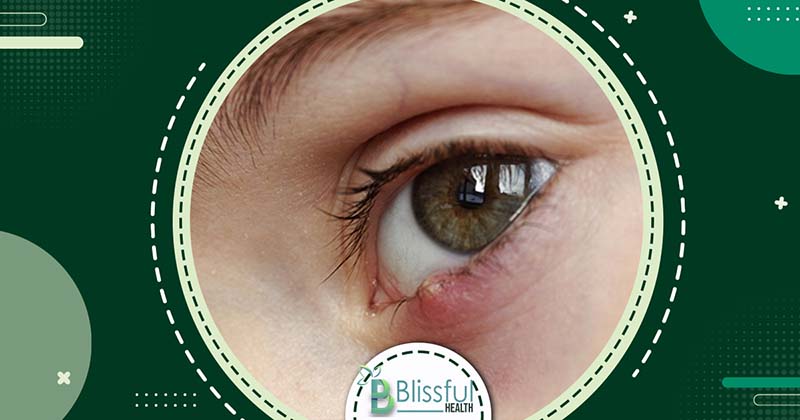
Find Out the Causes of Styes
Styes are primarily caused by an infection in the oil glands of the eyelid, with the most common culprit being the bacterium Staphylococcus aureus.
Other factors that can contribute to the development of styes include:
- Poor hygiene practices.
- Weakened immune system.
- Irritation of the eyelid from makeup or contact lenses.
- Hormonal changes, such as those occurring during pregnancy or menstruation, which can increase the risk of stye formation.
- Underlying conditions like blepharitis (eyelid inflammation) and rosacea (a skin condition affecting the face), which can make individuals more prone to developing styes.
Recognize Symptoms of Stye
The primary symptom of a stye is a painful red bump along the edge of your eyelid, near your eyelashes. Additional symptoms may include:
- Swelling of the eyelid, which can sometimes affect the entire eyelid.
- Discharge from the affected eye.
- Crusting along the eyelid.
- Sensitivity to light.
- Soreness and itching around the affected area.

- Excessive tearing of the eye.
- A scratchy sensation or the feeling that there’s something in your eye.
Treatment Options for Styes
Dealing with a stye can be both painful and bothersome. Here are some treatment options to help alleviate discomfort and speed up recovery:
- Hot Compresses: Applying hot compresses can help relieve pain and aid in clearing the infection. To make a hot compress, soak a piece of material (such as cotton balls) in hot water. Ensure it’s comfortably hot but not scalding. Apply the hot, wet material to the eyelid for several minutes, allowing it to cool. Repeat this several times a day to help the stye drain. It’s advisable for the person with the stye to manage this to minimize the risk of burns.

- Pain Relief: Over-the-counter pain relievers like paracetamol can help ease the pain associated with a stye.
- Antibiotic Treatment: In some cases, antibiotic ointments may be necessary to combat the infection. Occasionally, oral antibiotics may be prescribed by a healthcare professional if the stye is severe or persistent.
- Medical Intervention: If the stye doesn’t improve on its own, a doctor may need to open it up (lance it) to facilitate drainage.
- Seek Medical Attention: If the stye remains painful and hot after a few days, it’s essential to consult a doctor to assess the condition of the eye and determine the appropriate course of action.
It’s crucial to follow proper hygiene practices during stye treatment and avoid squeezing or attempting to pop the stye, as this can lead to further infection and complications.
Who Is at Risk of Getting a Stye?
Styes tend to occur more frequently in children than in adults, but they can appear at any age. If you have previously experienced a stye, your chances of developing another are higher.
Individuals with blepharitis, a persistent inflammation of the eyelid caused by blocked oil glands at the eyelash base, are also prone to styes. This condition can repeatedly irritate the eyelid and contribute to stye formation.
Furthermore, people suffering from diabetes or rosacea—a skin condition marked by redness—are more susceptible to styes. Although styes are not highly contagious, using personal items like towels or pillowcases that belong to someone with a stye can slightly increase your risk of getting one, though such instances are uncommon.
Stye Healing Process
While the exact progression of stye formation and healing can vary from person to person, there are general timelines to be aware of when discussing symptoms with your eye doctor.
Initial Symptoms (Days 1-2): Eyelid tenderness and swelling may occur without a visible bump during the first day or two.
Formation of Bump (Days 2-4): A small, red bump, often with a pustule or abscess, typically forms along the lash line around days two to four.
Pustule Drainage (Days 4-6): The pustule comes to a head and drains on its own, usually around days four to six.
Healing (Days 7-8): Once the pustule opens and drains, healing tends to progress rapidly, with the eyelid often fully healed by day seven or eight.
Chalazion Distinction: If the eyelid bump doesn’t develop a pustule and is closer to the center of the eyelid, it may be a chalazion instead of a stye. Chalazia are similar to styes but can last for months and typically aren’t infected.
How to Treat Stye at Home
Managing a stye at home involves following these dos and don’ts:
Do
- Use Warm Compresses: Apply a warm washcloth to your eyelid for 10 to 15 minutes, three to five times a day. Reheat the washcloth by soaking it in warm water, wringing it out, and repeating the process. Some find relief by using moistened green tea bags as eye compresses, as green tea contains antioxidants that may help kill bacteria.
- Clean Eyelids: Gently wipe away eye discharge with a mild solution made from half baby shampoo and half water. Alternatively, use eyelid wipes available in most drugstores to keep the area clean.
Don’t
- Squeeze or Pop the Stye: Avoid squeezing or popping the stye, as this can worsen the infection and lead to complications.
- Rub or Touch Your Eyelid: Refrain from rubbing or touching your eyelid to prevent spreading the infection or causing further irritation.
- Wear Makeup or Contact Lenses: Avoid wearing makeup or contact lenses until the stye has healed to prevent exacerbating the condition.
Following these guidelines can help alleviate symptoms and promote the natural healing process of the stye. If the stye persists or worsens despite home treatment, consult a healthcare professional for further evaluation and management.
When to Consult a Doctor About Styes
While styes typically improve on their own, there are instances when it’s important to seek medical attention:
- Lack of Improvement: If your stye doesn’t show signs of improvement within a few days despite home treatment, it’s advisable to consult a doctor for further evaluation and management.
- Presence of Blood in Drainage: If the drainage from the stye contains a significant amount of blood, it’s important to seek medical attention promptly.
- Rapid Growth: If the stye rapidly increases in size or shows signs of rapid growth, it could indicate a more serious issue that requires medical evaluation.
- Severe Swelling: Experiencing significant swelling around the stye or noticing new signs of infection warrants medical attention to prevent potential complications.
Increased swelling or the presence of new signs of infection should prompt immediate medical evaluation to ensure proper treatment and prevent further complications.

FAQ
How do I know if a stye is draining?
Once a stye starts draining, you may notice improvements in symptoms like pain and swelling. However, it’s essential to refrain from trying to pop or drain a stye yourself. Instead, seek treatment from a doctor to determine if incision and drainage are necessary.
What’s the worst that can happen from a stye in your eye?
In rare cases, the infection from a stye can spread to other areas around the eye, leading to a condition called periorbital cellulitis. Symptoms include swelling, pain, and redness around the eye, which require treatment with antibiotics.
How do I know if a stye is getting worse?
If you don’t see any improvements within a few days, notice the stye getting bigger, or experience worsening symptoms, it’s advisable to consult a doctor to assess if additional treatment is needed.
If I have an eye stye, how often should I change my pillowcase?
In most cases, you don’t need to change your pillowcase more frequently if you have a stye. However, bacteria can spread through contact with contaminated pillowcases or towels, especially if the stye is oozing. While rare, it’s best to avoid sharing pillowcases, towels, or bedsheets if you have a stye.
Conclusion
Stye eyes, caused by an infection in the glands or clogged eyelid follicles, is common in people who rub their eyes or use contact lenses incorrectly. Although they usually go away on their own and can be treated with warm compresses to speed up healing, styes that persist, impair vision, or bleed heavily should consult a doctor to avoid complications. Blissfulhealth will help you recognize the symptoms of a stye.